Authors: The Health and Reentry Project, in partnership with the Council on Criminal Justice and Waxman Strategies
In 2022, HARP recognized an opportunity to leverage Medicaid policy change to strengthen public health and safety by improving access to health care at reentry. To better understand goals for the development and implementation of potential policy change, HARP convened more than 70 stakeholders. Participants included state and federal Medicaid agency staff, managed care organizations, criminal justice leaders and advocates, social service and reentry provider organizations, current and former corrections officials, philanthropic organizations, academic researchers, racial justice advocates, formerly incarcerated individuals, and representatives of health care consumers and providers. HARP also interviewed experts and discussed these issues with a cross-sector Advisory Committee.
These diverse stakeholders reached clear consensus on what is needed, leading to the development of a new care model for successful reentry as well as guiding principles and essential actions for policy change. This care model, guiding principles, and essential actions continue to guide HARP’s work, informing our approach to how policies are developed and implemented and our practice of convening a wide range of stakeholders to understand priorities and operational realities.
HARP’s North Star: A New Care Model to Support Successful Reentry
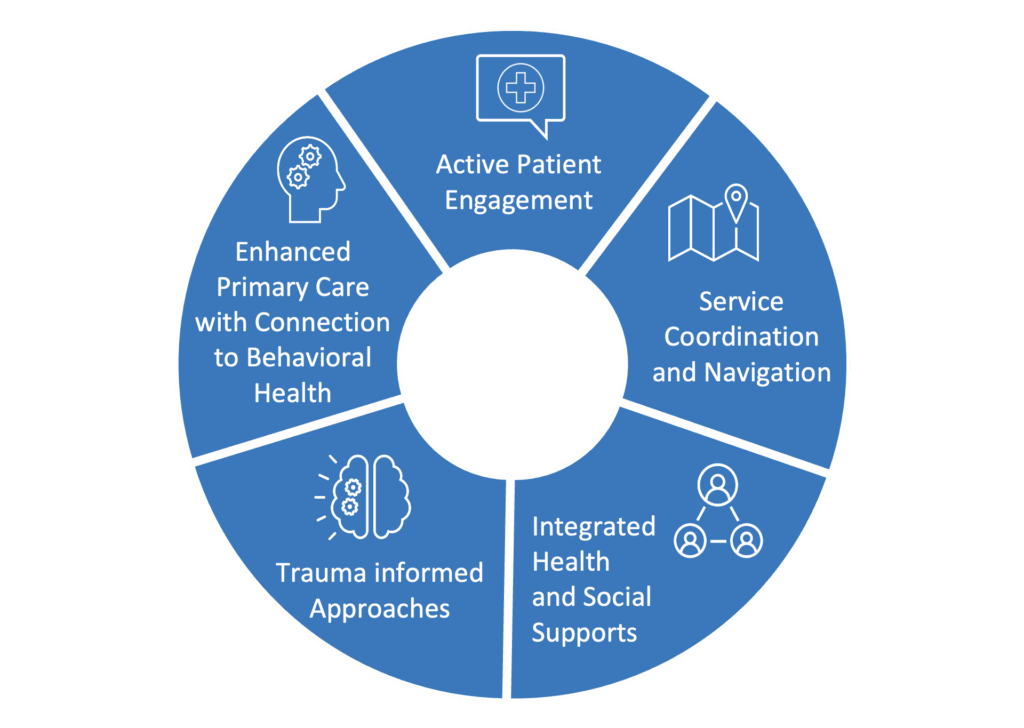
The convening participants identified six guiding principles for implementing changes to Medicaid’s role at reentry:
- Strengthen continuity of care of health care services before and after people leave prison and jail.
- Help people return to communities “healthy and whole” so they can be functional and successful community members.
- Advance equity to address significant racial and economic disparities that exist in justice system involvement, health service access, and health outcomes.
- Support evidence-based, clinical services rather than focus on correctional concerns, and involve people who have been under correctional control in policy development and implementation.
- Increase access to community services in order to potentially reduce reliance on the criminal justice system as a behavioral health service provider and strengthen continuity of care at reentry.
- Reinvest state and local savings generated by new policies in services including health care and community services, as well as services provided before release.
Convening participants also identified seven essential actions public officials should take as they translate Medicaid policy into effective practice:
- Align health care services provided in correctional settings with community-based standards of care.
- Account for key differences between prisons, jails, and juvenile justice facilities.
- Invest in systems and infrastructure to promote continuity and quality of care.
- Increase investments in community-based health care services.
- Strengthen the workforce to meet the needs of people leaving incarceration.
- Lead coordination between health, justice system, and directly impacted stakeholders.
- Commit to measuring and evaluating the impact of Medicaid policies.